“Live in the sunshine, swim the sea, drink the wild air” ~Ralph Waldo Emerson
There are plenty of good reasons to be outdoors this summer, and now we can add ‘safe haven’ to the list. As we all know, strict isolation strategies have been employed since mid-March to curb the spread of the pandemic. The resulting isolation, combined with fear of contagion and misinformation overload (“infodemic”) is creating a great deal of confusion and stress.[1]

There is no question that reducing the contact rate of latent individuals, and interventions such as quarantine and isolation, can effectively reduce the potential peak number of infections and delay the time of peak infection. However, as much as I believe this to be true as it applies to being indoors, I question whether being outdoors—even in groups—poses much risk at all. While there is still so much we don’t know about the virus transmission, we have yet to see proof or a strong likelihood that the outdoors poses a significant risk. In fact, research suggests it may be safer compared to indoors.
Staying Inside Versus Going Outside: Consider the Environment
Consider this: The hot spots for the virus have been centered on nursing homes, meat factories, prisons, and hospitals, where people are indoors in close contact for extended periods of time. But beaches and parks were closed for fear of people crowding together without any evidence that the virus could spread outdoors. In fact, no outdoor activities have been shown to be vectors for the spread of COVID-19. A recent study examined hundreds of outbreaks and traced only one to an outdoor environment. [2]
A study from four Chinese scientists suggests that COVID-19 is much more likely to spread indoors than outdoors. The proctors reviewed more than 1,000 COVID-19 cases in China, classified groups of cases into “clusters” and “outbreaks,” and summarized their findings: “We identified only a single outbreak in an outdoor environment, which involved two cases. The first salient feature of the 318 identified outbreaks that involved three or more cases is that they all occurred in indoor environments.”2
Studies are mounting that suggest activities held outdoors as temperatures warm pose much lower risk of viral spread than those in confined indoor spaces. Sunlight, humidity, wind, and other natural forces work to rapidly decay and disperse the virus. These environmental factors suggest that it would be wise to move indoor events to outside whenever possible. These include church gatherings, weddings, sporting events, restaurants, family meals, and even business meetings.

Hartford, Connecticut is one of the cities exploring allowing restaurants to expand their outdoor seating options into parking lots or other outdoor spaces. Closing streets to cars and allowing pedestrian traffic only would create more safe outdoor seating.
In addition to the minimal (if any) virus risk involved in pursuing outdoor activities, it’s important to acknowledge the negative effects of being isolated indoors on our physical, mental, and emotional wellbeing. A significant consequence of quarantine is a change in lifestyle, which is reflected in reduced physical activity and an unhealthy diet.[3]
During the pandemic, we’ve been encouraged to isolate ourselves indoors as much as possible, while rigorously disinfecting household surfaces. Both practices contribute to poor respiratory health. The indoor air temperatures of most buildings are a potential factor contributing to virus spread in most residential homes as well as in public buildings. And with the summer months coming, air conditioning without proper filtration can worsen the situation.[4]
Instead of using toxic cleaning substances multiple times a day, I suggest the simple measure of increasing the movement of fresh air. Open windows and doors whenever possible, and use fans to increase ventilation.
In rooms with little to no fresh air circulating, viral particles can easily linger outside a six-foot radius. But outdoors, especially with a breeze blowing, I don’t believe the same social distancing requirement should apply. The recent proof of aerosolized droplets being able to travel well over six feet supports the question of whether our current social distancing guidelines are even adequate in an indoor environment. I suggest that we use common sense. Obviously, you want to stay away from crowded situations, both indoors and outdoors.
“All truths are easy to understand once they are discovered; the point is to discover them.” ~Galileo
Outdoor Enthusiasts Are Not the Real Threat
There are those who scold and shame anyone who dares to go out to get a little exercise and fresh air. I maintain that surfers, swimmers, runners, hikers, walkers, and bikers are the least of our worries. Personally, I don’t understand why parks have been shut down throughout the United States, and the closures at times enforced with rigor. Tom Brady was chased from a closed Tampa Bay park after he was discovered working out, apparently alone. A father in Colorado was briefly detained by police for playing t-ball with his 6-year-old daughter on a softball field. A sure sign of fanaticism is the inability to make distinctions between risky and non-risky activities and between places hard-hit and places not.[5]

Spend Time in the Forest to Improve Your Health
“Let the heavens be glad, and let the earth rejoice; let the sea roar, and all that fills it; let the field exult, and everything in it! Then shall all the trees of the forest sing for joy.” – Psalm 96: 11-12
A quiet, peaceful walk through the woods, surrounded by beautiful scenery, clean air, and the scent of pines and junipers…it’s no wonder that we respond positively to forest environments.
Now, ‘Forest Medicine’ has actually become a science, combining alternative medicine, environmental medicine and preventive medicine. Forest environments have demonstrated the following beneficial effects on human health:

1. Increased human natural killer (NK) activity, the number of NK cells, and the intracellular levels of anti-cancer proteins, suggesting a preventive effect on cancers.
2. Reduced blood pressure, heart rate, and stress hormones, such as urinary adrenaline and noradrenaline and salivary cortisol.
3. Increased activity of parasympathetic nerves and reduced activity of sympathetic nerves.
4. Increased levels of serum adiponectin and dehydroepiandrosterone sulfate.
5. In the Profile of Mood States (POMS) test, reduced scores for anxiety, anger, fatigue, and confusion, and increased scores for vigor.6
For more evidence of the benefits of spending time in forests, consider this 2010 study, which found that 2-night/3-day trips to forest parks enhanced human natural killer (NK) NK activity, the number of NK cells, and intracellular anti-cancer proteins in lymphocytes, and that this increased NK activity lasted for more than 7 days after the trip in both male and female subjects.7
As an herbalist, I find it particularly interesting that research has found compounds called phytoncides released from trees decreases stress hormone levels and may partially contribute to the increased NK activity.8
Finally, according to a study published in 2011 that compared the effects of walking the streets of a city to go for a hike, or walking in nature among the trees and plants, the day trip to the forest park significantly reduced blood pressure and urinary noradrenaline and dopamine levels and significantly increased serum adiponectin and dehydroepiandrosterone sulfate (DHEA-S) levels. The same was not true for city walks.9
Forrest walking as the added advantage of breathing cleaner air, over walking in the city. COVID-19 spreads more in higher polluted area, compared to lower polluted areas.10
The Need for Human Connection
During the COVID-19 pandemic, numerous healthcare workers have committed suicide in a tragedy that has touched all continents.Many of us know of people—perhaps even ourselves—who have suffered the devastating effects of social isolation.
We all think we know how to take good care of ourselves. We eat our veggies, exercise, and try to get enough sleep. But how many of us know that human social connection is just as critical? Human-to-human connection can significantly improve physical, mental, and emotional well-being, and can even help our immune systems.
In studying the Blue Zones—the healthiest places in the world—researchers have noted that one of the most consistent findings is the important of social connection.
Strong social connection is associated with:
–50% increased chance of longevity
– strengthening your immune system, and
– helping you recover from disease faster
According to a pooled analysis of 148 studies, the influence of social relationships on risk for mortality is stronger than other well-established risk factors for mortality.11

Social Relationships and Mortality Risk: A Meta-analytic Review
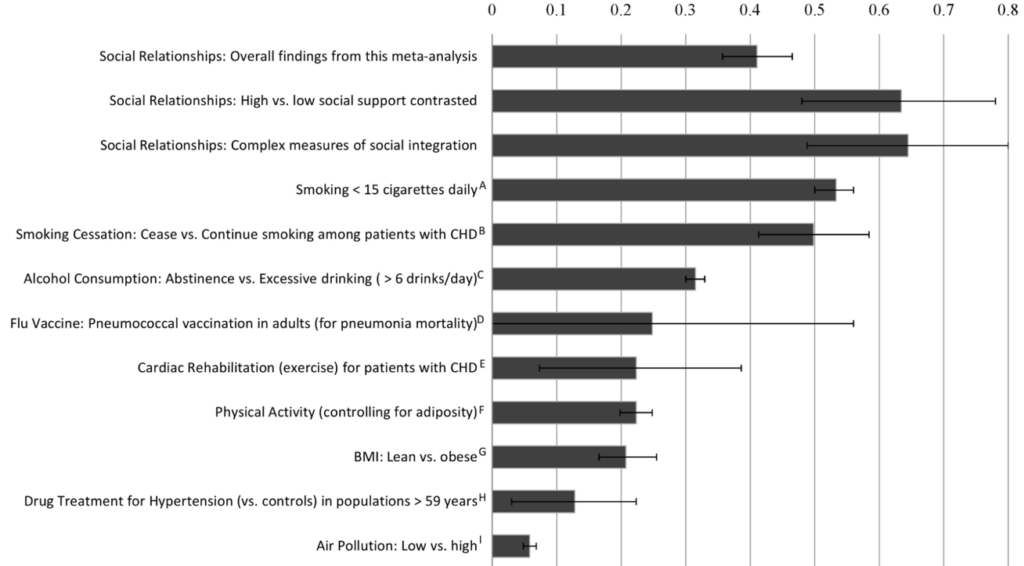
11
Psychological researchers George Slavich and Steven Cole of the University of California, Los Angeles discovered that certain genes can be “turned on” and “turned off” by different social-environmental conditions, especially our subjective perceptions of those conditions.12
One of the most important medical discoveries of the past two decades has been that the immune system and inflammation are involved in not just a few select disorders, but a wide variety of mental and physical health problems that dominate present-day morbidity and mortality worldwide.13
My advice is to not avoid being outdoors, and to not be afraid of interacting with a carefully chosen circle of friends and family. Use common sense and connect. There are many ways to be with people that are not risky—go for walks together, eat a meal outdoors, or gather together in a circle outside and socialize.
“A smile is a curve that sets everything straight” ~Phyllis Diller
Sunlight is an Effective Disinfectant for Surfaces
Did you know that natural sunlight might be one of the most effective disinfectants to SARS-CoV-2? Previous studies have demonstrated that SARS-CoV-2 is stable on surfaces for extended periods under indoor conditions.
A recent study found that simulated sunlight rapidly inactivated SARS-CoV-2 suspended in either simulated saliva or culture media and dried on stainless steel coupons. Ninety percent of infectious virus particles were inactivated every 6.8 minutes in simulated saliva and every 14.3 minutes in culture media when exposed to simulated sunlight representative of the summer solstice at 40oN latitude at sea level on a clear day. Significant inactivation also occurred, albeit at a slower rate, under lower simulated sunlight levels. This study provides the first evidence that sunlight may rapidly inactivate SARS-CoV-2 on surfaces.14

How Useful Are Masks?
According to a recent study, neither surgical nor cotton masks effectively filter SARS–CoV-2 from coughs of infected patients. The SARS–CoV particle from the 2002–2004 outbreak was estimated as 0.08 to 0.14 μm; assuming that SARS-CoV-2 has a similar size, surgical masks are unlikely to effectively filter this virus.15
However, other studies show that wearing masks can be helpful, including at home. In a retrospective cohort study, researchers in China found that wearing masks at home appeared to help prevent pre-symptomatic COVID-19 cases from infecting family members. When at least one household member wore a facemask—which could be the infected person or an uninfected family member. Prior to anyone showing symptoms, odds of within-family transmission were cut 79% (OR 0.21, 95% CI 0.06-0.79).16
In a reversal of their previous recommendations, the World Health Organization (WHO) advises using masks in communities, during home care, and in health care settings in areas that have reported cases of COVID-19.
Although WHO cautions that a mask alone does not provide an adequate level of protection, they are encouraging the general public to wear masks in specific situations such as areas with “known or suspected widespread transmission and limited or no capacity to implement other containment measures such as physical distancing, contact tracing, appropriate testing, isolation and care for suspected and confirmed cases.” However, they also note that although many countries have recommended the use of fabric masks for the general public, “the widespread use of masks by healthy people in the community setting is not yet supported by high quality or direct scientific evidence.” 17
Ironically, wearing a mask can potentially increase risk, due to self-contamination. Facemasks are generally not comfortable to wear, and people tend to adjust them frequently. This creates more opportunity for the virus to be spread to the eyes, nose, and mouth when the face is touched with contaminated hands.
A 2015 study published in the British Medical Journal cautioned against the use of cloth masks in high-risk situations. Researchers found that moisture retention, the reuse of cloth masks, and poor filtration may result in increased risk of infection. Clinical respiratory illness and influenza-like illness were significantly higher in the cloth masks group compared with the medical masks group.18,19
A systematic review of randomized controlled clinical trials on use of respiratory protection by healthcare workers, sick patients and community members was conducted. A total of 19 randomized controlled trials were included in this study – 8 in community settings, 6 in healthcare settings and 5 as source control. Randomized controlled trials in health care workers showed that respirators, if worn continually during a shift, were effective but not if worn intermittently. Medical masks were not effective, and cloth masks even less effective.20
With all the conflicting evidence and recommendations, whom should we believe, and what should we do? In evaluating all the studies—and using common sense—I believe masks can be helpful in reducing how far aerosol droplets may travel during breathing, speaking, singing, sneezing, or coughing. For the same reasons, you should cover your mouth or nose with your forearm, the inside of your elbow, or with a tissue when sneezing.
Guidelines for Staying Safe and Healthy in These Challenging Times
In an attempt to present a rational approach to summer activities, I suggest the following:
- Be outdoors in nature whenever possible, and deeply breathe in the fresh air and enjoy the sunshine. When we unite with nature, we are nourished throughout our bodies, minds, and spirits.
- When indoors, open the windows to get fresh air and cross ventilation.
- Do not keep the air conditioner too low and try to maintain the indoor temperature at or reasonably close to the outside temperature.
- Wear a mask indoors when there is potential prolonged exposure to other people, especially when ventilation is poor.
- Widen your circle little by little to include other people. Don’t be overly fearful or emotional, but be thoughtful, understanding and rational.
Making Peace with Everything, Including Viruses
This may be blasphemy for some, but I believe that a state of true health requires making peace with everything, including COVID-19. Viruses have been part of the world, and of us since the beginning of time. One thing we have learned from studying longevity is that in general, people that live long and healthy lives have been minimally exposed to industrialized environments but highly exposed to a variety of microbes, including viruses. Microbial diversity is now recognized as a significant component of disease resilience and good health.21
Viruses form mutually beneficial relationships with animals and sometimes, even humans. This relationship is more complex in plants, as well, where some viruses actually aid in drought and frost protection.
This doesn’t mean when a new invading bug comes into our ecosystem, such as COVID-19, we don’t need to put it in its place. But when we try to control a virus by isolating ourselves and disinfecting everything in our path, we are creating an environment conducive to viral takeover. Instead, I propose that we need to focus on building health and our innate immunological strength. We must always remember that adaptation is the single most important factor in health and longevity.
“The sun,–the bright sun, that
brings back, not light alone, but new life, and hope, and freshness to
man–burst upon the crowded city in clear and radiant glory. Through costly-colored
glass and paper-mended window, through cathedral dome and rotten crevice, it
shed its equal ray.” ~Charles Dickens, Oliver Twist

REFERENCES
[1] Burtscher J, Burtscher M, Millet GP. (Indoor) isolation, stress and physical inactivity: vicious circles accelerated by Covid 19? . Scand J Med Sci Sports. 2020;10.1111/sms.13706. doi:10.1111/sms.13706
[2] Hua Qian, Te Miao, Li LIU, Xiaohong Zheng, Danting Luo, Yuguo Li medRxiv 2020.04.04.20053058; doi: https://doi.org/10.1101/2020.04.04.20053058
[3] Mattioli AV, Ballerini Puviani M, Nasi M, Farinetti A. COVID-19 pandemic: the effects of quarantine on cardiovascular risk [published online ahead of print, 2020 May 5]. Eur J Clin Nutr. 2020;1‐4. doi:10.1038/s41430-020-0646-z
[4] Amoatey P, Omidvarborna H, Baawain MS, Al-Mamun A. Impact of building ventilation systems and habitual indoor incense burning on SARS-CoV-2 virus transmissions in Middle Eastern countries . Sci Total Environ. 2020;733:139356.
[5] Lowery, R., Stop slamming surfers, bikers: No evidence outdoor activities pose coronavirus risks, April 23, 2020; https://nypost.com/2020/04/23/no-evidence-outdoor-activities-pose-coronavirus-risks/, Retrieved 5/21/2020
6 Li Q. Effets des forêts et des bains de forêt (shinrin-yoku) sur la santé humaine : une revue de la littérature [Effect of forest bathing (shinrin-yoku) on human health: A review of the literature]. Sante Publique. 2019;S1(HS):135‐143. doi:10.3917/spub.190.0135
7 Li Q, Morimoto K, Kobayashi M, et al. A forest bathing trip increases human natural killer activity and expression of anti-cancer proteins in female subjects. J Biol Regul Homeost Agents. 2008;22(1):45‐55.
8 Li Q, Kobayashi M, Inagaki H, Hirata Y, Li YJ, Hirata K, Shimizu T, Suzuki H, Katsumata M, Wakayama Y, Kawada T, Ohira T, Matsui N, Kagawa T. A day trip to a forest park increases human natural killer activity and the expression of anti-cancer proteins in male subjects.
J Biol Regul Homeost Agents. 2010 Apr-Jun;24(2):157-65.
9 Li Q, Otsuka T, Kobayashi M, et al. Acute effects of walking in forest environments on cardiovascular and metabolic parameters. Eur J Appl Physiol. 2011;111(11):2845‐2853. doi:10.1007/s00421-011-1918-z
10 Zoran MA, Savastru RS, Savastru DM, Tautan MN. Assessing the relationship between surface levels of PM2.5 and PM10 particulate matter impact on COVID-19 in Milan, Italy [published online ahead of print, 2020 Jun 2]. Sci Total Environ. 2020;738:139825. doi:10.1016/j.scitotenv.2020.139825
11 Holt-Lunstad J, Smith TB, Layton JB (2010) Social Relationships and Mortality Risk: A Meta-analytic Review. PLoS Med 7(7): e1000316. https://doi.org/10.1371/journal.pmed.1000316
12 Slavich GM, Cole SW. The Emerging Field of Human Social Genomics. Clin Psychol Sci. 2013;1(3):331‐348. doi:10.1177/2167702613478594
13 Furman D, Campisi J, Verdin E, et al. Chronic inflammation in the etiology of disease across the life span. Nat Med. 2019;25(12):1822‐1832. doi:10.1038/s41591-019-0675-0
14 Ratnesar-Shumate S, Williams G, Green B, et al. Simulated Sunlight Rapidly Inactivates SARS-CoV-2 on Surfaces [published online ahead of print, 2020 May 20]. J Infect Dis. 2020;jiaa274. doi:10.1093/infdis/jiaa274
15 Zamora JE, Murdoch J, Simchison B, Day AG. Contamination: a comparison of 2 personal protective systems. CMAJ. 2006;175(3):249-54.
16 Kwon JH, Burnham CD, Reske KA, Liang SY, Hink T, Wallace MA, et al. Assessment of Healthcare Worker Protocol Deviations and Self-Contamination During Personal Protective Equipment Donning and Doffing. Infect Control Hosp Epidemiol. 2017;38(9):1077-83.
17 https://www.who.int/publications/i/item/advice-on-the-use-of-masks-in-the-community-during-home-care-and-in-healthcare-settings-in-the-context-of-the-novel-coronavirus-(2019-ncov)-outbreak, retrieved June 8th, 2020.
18 MacIntyre CR, Seale H, Dung TC, et al. A cluster randomised trial of cloth masks compared with medical masks in healthcare workers. BMJ Open. 2015;5(4):e006577. Published 2015 Apr 22. doi:10.1136/bmjopen-2014-006577
19 Li DTS, Samaranayake LP, Leung YY, Neelakantan P. Facial protection in the era of COVID-19: a narrative review [published online ahead of print, 2020 Jun 7]. Oral Dis. 2020;10.1111/odi.13460. doi:10.1111/odi.13460
20 MacIntyre CR, Chughtai AA. A rapid systematic review of the efficacy of face masks and respirators against coronaviruses and other respiratory transmissible viruses for the community, healthcare workers and sick patients [published online ahead of print, 2020 Apr 30]. Int J Nurs Stud. 2020;108:103629. doi:10.1016/j.ijnurstu.2020.103629
21 Sonnenburg ED & Sonnenburg JL The ancestral and industrialized gut microbiota and implications for human health. Nat. Rev. Microbiol 17, 383–390 (2019).


One Reply to “The Courage to Step into the Great Outdoors”