Do multiple COVID-19 vaccines weaken the immune system?
We’re indeed all trying to put the pandemic behind us. Despite this, I think it’s important not to ignore new research that sheds light on the ongoing debates surrounding COVID-19, both the virus itself and the mRNA vaccines.
I made a personal choice not to get vaccinated.
My decision was based on three factors:
1. I consider myself extremely healthy. What’s more, I have none of the health factors that put me at risk for severe infection, and I am not operating from a position of fear.
2. I have complete faith in herbal and nutritional medicine to provide the immune support my body needs to effectively manage and overcome the virus if I were to get sick.
3. I didn’t feel comfortable taking the current vaccines without more high-quality data.
Our health authorities urged—or even required—everyone to get these vaccines. However, since the beginning of the concern over COVID-19, I have been reading and analyzing the science.
For nearly as long as public health has been sounding the alarm, there has been more we don’t know than we do know about these injections’ safety, efficacy, and necessity. There is a greater extent of unknowns than certainties.
Making The Right Health Decisions
How do you make the right health decision? I make health decisions based first on wisdom, then on knowledge, and finally, on prayer.
Wisdom comes from modern science but also from ancient medical models, including traditional Chinese medicine, Ayurvedic medicine, and even our American traditions such as Eclectic Medicine. These systems of medicine offer different philosophical approaches to health and healing. But they all have something in common: they posit that the most important thing we can do to strengthen our body’s general resistance to diseases and toxins and our overall vitality is to build robustness.
Being informed by this wisdom, I then seek to understand the Western perspective and knowledge. This means reviewing all the relevant science regarding any given issue.
Finally, before I decide what to do, I try to sit quietly in meditation and prayer, getting in touch with my deepest intuition and asking for guidance from the “divine.”
New Study: Repeated COVID-19 Vaccines Weaken the Immune System
While I was working on deciding if the COVID-19 vaccines are effective, a recently published study came to my attention. This peer-reviewed science found that the more COVID-19 vaccines a person receives, the more weakened their immune system becomes.
In other words, repeated COVID-19 vaccines weaken the immune system.
The international team of researchers, writing in the peer-reviewed journal Vaccines, proposed the mechanism by which repeated COVID-19 vaccines weaken the immune system: multiple vaccines cause a spike in the production of IgG4 antibodies within the vaccine recipient’s body.
As the researchers themselves explain:
The repeated doses of mRNA vaccines for COVID-19 result in increased proportions of anti-spike antibodies of the IgG4 subclass, which are known to neutralize well and to form mixed immune complexes with IgG1 but, in a pure form, might be less effective than IgG1 or IgG3 antibodies in facilitating opsonization by phagocytes, complement fixation, and NK cell-dependent elimination of infected cells.
IgG4 Antibodies
These IgG4 antibodies are not benign. In fact, their presence can lead to a plethora of problems for the human body, including cancer, organ dysfunction, organ failure, and even death.[1]
In another recent paper published in Science Immunology, a team of German scientists showed that administering three doses of an mRNA vaccine encoding the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) spike antigen eventually results in an increased proportion of antigen-specific antibodies of the immunoglobulin G4 (IgG4) subtype, but IgG4 antibodies were not induced after an adenoviral vector vaccine.[2]
What could possibly be wrong with increased IgG4?
IgG4 is a unique antibody in the human body.
Human IgG4 makes up about 3 to 6% of all human IgG and remains poorly understood from an evolutionary and functional standpoint.
Human IgG4 molecules can be useful as a noninflammatory choice of antibody framework when engineering “blocking” therapeutic antibodies. However, this antibody subclass appears to weaken or deplete specific circulating immune cells generally essential for a well-rounded, healthy immune system.
Human IgG4 molecules negatively impact antibody-dependent cellular cytotoxicity (ADCC) by natural killer (NK) cells to be poorly facilitated.
NK cells are important as a first-line defense against viral infections and are essential for cancer prevention and treatment.[3],[4]
Specifically, IgG4 antibodies do not bind well to activating Fc receptors and to C1q. As a result, they do not activate complement effectively, and opsonization and ADCC are compromised.[5]
Similar results were observed in yet another contemporaneous study by another group of scientists.[6] This group of researchers found that mRNA vaccines increase long-term IgG4 responses compared to adenovirus-based vaccines. These results provoke a reconsideration of some fundamental immune mechanisms unique to the human immune system.
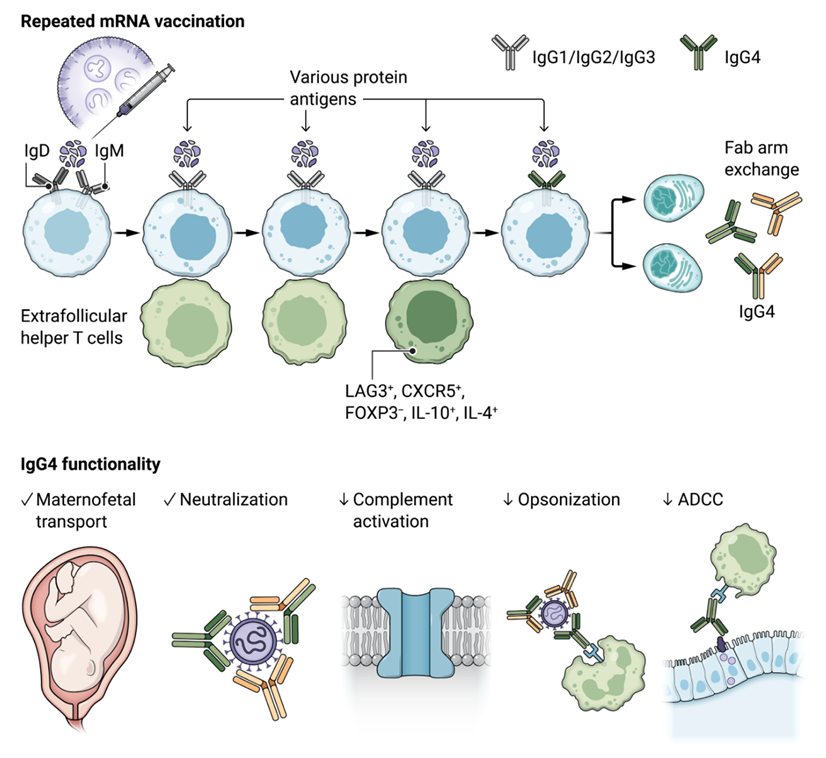
The top panel depicts the induction of IgG4 by persistent antigen (or repeated doses of a protein or glycoprotein immunogen) and by extrafollicular T helper cells that secrete IL-10 and IL-4. The IgG4 molecule shown at the bottom right of the top panel has undergone “Fab arm exchange.” The bottom panel depicts the functionality of human IgG4 relative to other human IgG subclasses. Although IgG4 is efficiently transported across the placenta and neutralizes with high efficiency, IgG4 antibodies do not bind well to activating Fc receptors and to C1q. As a result, they do not activate complement effectively, and opsonization and ADCC are compromised. CREDIT: A. FISHER/SCIENCE IMMUNOLOGY
Another recent study examined possible non-specific effects of the novel COVID-19 vaccines.
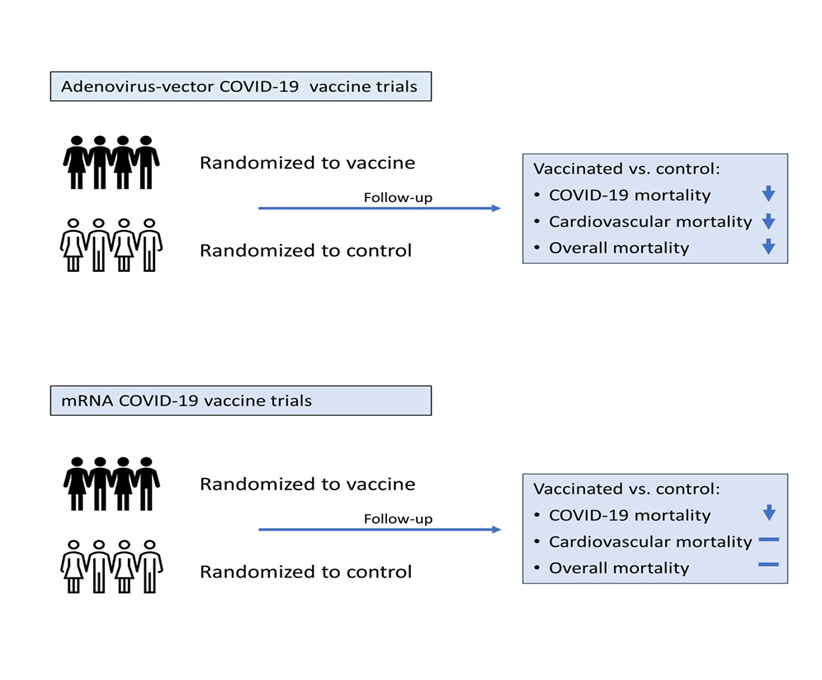
This study reviewed randomized control trials of mRNA and adenovirus-vector COVID-19 vaccines. The researchers calculated mortality risk ratios for people who received mRNA COVID-19 vaccines compared to people who received a placebo.
“The differences in the effects of adenovirus-vector and mRNA vaccines on overall mortality, if true, would have a major impact on global health,” the research team wrote in their conclusion.
“If validated in additional studies, the protective non-specific effects of adenovirus-based vaccines on non-COVID-19 mortality, in addition to their effectiveness against SARS-CoV-2 infection, may represent an important advantage in vulnerable populations in which cardiovascular mortality is high.”
However, they continue: “Ironically, the rich countries in Europe and the USA have emphasized the more expensive mRNA vaccines because of slightly better short-term vaccine efficacy against COVID-19 compared to the relatively inexpensive adenovirus-vector vaccines.”[7]
So, despite marked differences in vaccine-induced antibody responses, no significant difference in spike receptor binding domain (RBD)-specific B cell frequencies and interferon-gamma-secreting T cell levels were observed between mRNA-vaccinated and adenoviral vector-vaccinated individuals.[8]
COVID-19 Vaccines weaken the immune system: highlights on vaccines and overall survival rates
- We don’t yet really know or understand if COVID-19 vaccines have non-specific effects on overall survival, though several peer-reviewed studies suggest that the vaccines themselves may be as dangerous or even more dangerous—especially for young people—than the virus
- The randomized trials of mRNA and adenovirus vaccines had information on deaths
- The relative mortality risk for mRNA vaccine vs. placebo was 1.03 (0.63–1.71)
- For the adenovirus vaccine vs. placebo, it was significantly different: 0.37 (0.19–0.70)
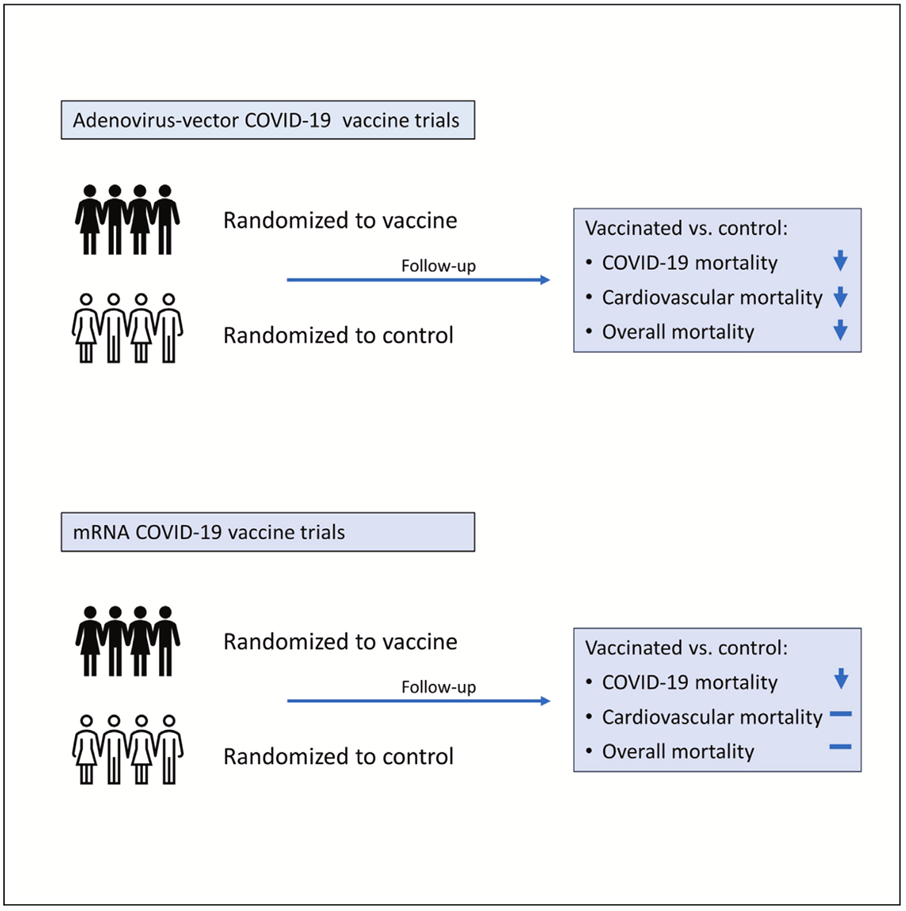
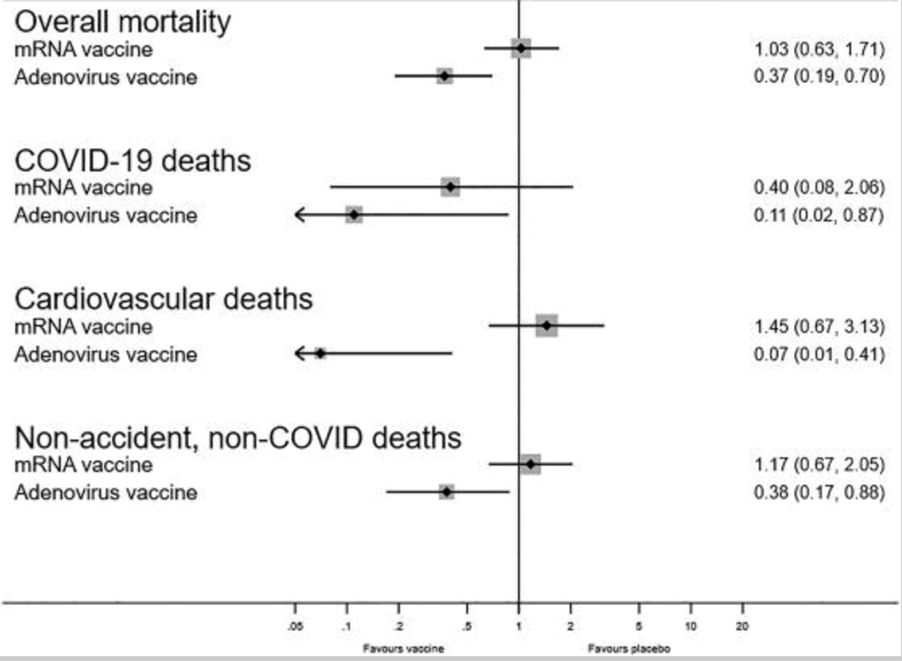
In the randomized control trials with the longest possible blinded follow-up, mRNA vaccines had no effect on overall mortality despite appearing to protect against some COVID-19 deaths.
At the same time, adenovirus-vector vaccines appear to be associated with lower overall mortality.[9]
What does all of this mean? Have we been giving—even forcing—everyone to take a vaccine that is experimental, likely ineffective, and even potentially harmful based solely on the fact that it induces a quicker immune response without looking at its long-term impact on the immune system?
Support Our Immune Systems
As my regular readers are aware, I believe it is important to restore the strength of our immune systems through the utilization of adaptogenic formulas and immune-building tonic formulations. Accompanying this approach, achieving balance in zinc, vitamin D, and selenium levels is crucial. Furthermore, incorporating a variety of plant foods in our diets, along with some traditional fermented foods, can foster the development of a diverse and beneficial microbiome.
Why is this kind of immune support important? Because at least one study has found that fecal microbiota alterations are associated with fecal levels of SARS-CoV-2 and COVID-19 severity.
This study provides us with valuable insight indicating that adopting a whole-food, plant-based diet can positively influence the composition of the intestinal microbiota, which in turn can reduce the severity of various diseases.[10]If multiple COVID-19 vaccines weaken the immune system, as the research appears to indicate, we must explore alternative strategies for evading the virus. Rather than getting an escalation series of booster vaccines , we can bolster the immune system by implementing botanical and nutritional medicine and adjusting our dietary habits and lifestyle choices.
About the Author:
Donald R. Yance is the founder of the Mederi Center. A Clinical Master Herbalist and Certified Nutritionist, Donnie is renowned for his extraordinary knowledge and deep understanding of the healing properties of plants and nutrition, as well as of epigenetics, laboratory medicine, oncologic pathology, and molecular oncology. He is a professional member of the American Herbalists Guild, National Association of Nutrition Professionals, Academy of Integrative Health and Medicine, and the Society for Integrative Oncology.
References:
[4] Wolf, N.K., Kissiov, D.U. & Raulet, D.H. Roles of natural killer cells in immunity to cancer, and applications to immunotherapy. Nat Rev Immunol 23, 90–105 (2023). https://doi.org/10.1038/s41577-022-00732-1
[6] J. S. Buhre, T. Pongracz, I. Künsting, A. S. Lixenfeld, W. Wang, J. Nouta, S. Lehrian, F. Schmelter, H. B. Lunding, L. Dühring, C. Kern, J. Petry, E. L. Martin, B. Föh, M. Steinhaus, V. von Kopylow, C. Sina, T. Graf, J. Rahmöller, M. Wuhrer, M. Ehlers, mRNA vaccines against SARS-CoV-2 induce comparably low long-term IgG Fc galactosylation and sialylation levels but increasing long-term IgG4 responses compared to an adenovirus-based vaccine. Front. Immunol. 13, 1020844 (2023).
[10] Zuo T, Zhang F, Lui GCY, Yeoh YK, Li AYL, Zhan H, Wan Y, Chung ACK, Cheung CP, Chen N, Lai CKC, Chen Z, Tso EYK, Fung KSC, Chan V, Ling L, Joynt G, Hui DSC, Chan FKL, Chan PKS, Ng SC. Alterations in Gut Microbiota of Patients With COVID-19 During Time of Hospitalization. Gastroenterology. 2020 Sep;159(3):944-955.e8. doi: 10.1053/j.gastro.2020.05.048. Epub 2020 May 20. PMID: 32442562; PMCID: PMC7237927.


Thank you for your insights. But what do we do if we already had the vaccine and one booster?
Finally, these negative outcomes are not expected to affect all people who have received these mRNA vaccines. Individuals with genetic susceptibility, immune deficiencies, and comorbidities are probably the most likely to be affected. However, this gives rise to a disturbing paradox—if people who are the most affected by the COVID-19 disease (the elderly, diabetics, hypertensive, and immunocompromised people like those with HIV) are also more susceptible to suffering the negative effects of repeated mRNA vaccination, is it then justified to booster them? As Omicron subvariants have been demonstrated to be less pathogenic [133,134,135,136,137], and mRNA vaccines do not protect against re-infection [14,138], clinicians should be aware of the possible detrimental effects on the immune system by administering boosters.
This information is disconcerting and not surprising given what’s been coming to light over the last couple of years. As an allopathic physician I had to get the vaccine to be able to work.
Are there botanical solutions to mitigate potential damage from these vaccines?
Thank you so much for your wise and balanced insights. We seem to think a lot alike. I hope we bump into each other sometime!
I like your emphasis on promoting biological vitality in the individual through botanical medicine and lifestyle/diet modifications. I also like how you fuse this philosophy with current scientific input. I also value contemplative prayer as one the main ways I make any decision in life (including whether or not I take a vaccine.)
Thankfully I am in private practice and my job has not been in at risk regarding what should be a personal decision about a vaccine. I have unfortunately had some patients (mostly nurses) who have lost their jobs over this decision. This should never happen.
Bert Mathieson, ND
New Hampshire Natural Health Clinic
Bedford, NH
Thank you so much Donnie – always appreciate and learn from your comprehensive studies and data-filled articles.